Flow Cytometry Quantifying Legionella in Shorter Time
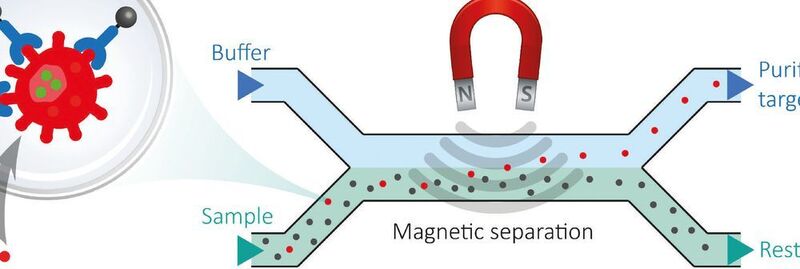
Identifying the source of infection is essential for taking action in outbreaks of Legionnaire's disease. The combination of immunomagnetic separation and flow cytometry delivers precise results in less than two hours and knows virtually no limits to the variety of applications.
Related Vendor
Legionella were not discovered and described until 1976. At that time, a mysterious pneumonia affected numerous participants during a congress of the American Legion, a veteran's association. After a feverish search, doctors microbiologists identified the infectious agent causing for this “Legionnaire’s disease” and named it Legionella [1].
In contrast to other bacteria, Legionella are comparatively heat-resistant and prefer to multiply at temperatures between 25 °C and 45 °C. Through the establishment of hot water systems, air conditioners or whirlpools, they seem to have found an ecological niche that renders them a serious health hazard. Infection occurs by inhaling aerosols, which are produced in the shower or in air-conditioning systems. But also decorative fountains, for example, have already been identified as a source of infection. It is estimated that 10,000 cases of life-threatening Legionnaires' pneumonia occur annually in Europe. The lethality rate averages 10% [2]. Outbreaks are particularly serious if they occur in hospitals, retirement homes or hotels.
The largest outbreak of Legionnaires' disease in Germany to date occurred in Warstein in 2013. Investigations have shown that the activated sludge basin of a wastewater treatment plant was highly contaminated with Legionella. Via a river, the bacteria reached industrial recooling plants and from there were distributed into the environment via aerosols. A total of 165 cases of illness and suspected cases had been reported [6]. In Switzerland the number of cases of Legionnaire's disease increased by 35% since 2016. The Swiss government wants to stop the epidemic with a task force [18]. In the US it is the state of New York that leads the nation a 38% increase in cases compared with 2016. Of the state total, New York City recorded 441 cases — a 65% increase over 2016.
The fact that the source of an outbreak can often only be identified after about two weeks, if at all, since the analysis is time-consuming and prone to errors, contributes to the fact that so many cases have occurred.
Questioning the standard procedure
The established standard method for Legionella detection, ISO 11731 [7], is based on the cultivation of bacteria on agar plates, which leads to variable results and takes up to 14 days [8-10]. An extensive round robin test between different laboratories in the USA has also shown that the concentration of Legionella can be dramatically underestimated using plating methods [11]. One reason for this is that not all bacterial cells present and alive in a given sample will grow on agar medium [12]. Therefore, the standard method does not detect these cells. Especially after stagnation and chemical or thermal disinfection, such cells, called VBNC — viable but non-culturable cells — occur more frequently. Since the efficiency of disinfection measures is assessed using the standard method, the microbiological results are difficult to interpret [13, 14]. It is therefore not surprising that very high levels of Legionella are often measured weeks after disinfection measures have been carried out [4, 15].
(ID:45099527)





:quality(80)/p7i.vogel.de/wcms/d6/25/d625408f8628b90bf08a73d0c6d57fe7/0131163821v2.jpeg)
:quality(80)/p7i.vogel.de/wcms/0e/72/0e7296d4ca7d79eb7b3e4f668641af8f/0131148508v2.jpeg)
:quality(80)/p7i.vogel.de/wcms/6b/9a/6b9a2f9d820c458d6518f7d3c0cc990e/0131057985v2.jpeg)
:quality(80)/p7i.vogel.de/wcms/ed/07/ed0756a2495cf3591db2f3c23bedd39c/0131055520v2.jpeg)
:quality(80)/p7i.vogel.de/wcms/52/2e/522e60883334ab2d806e6038a11e9204/0131030069v3.jpeg)
:quality(80)/p7i.vogel.de/wcms/06/0e/060e08234d208d1faca16ad0cf582ff3/0131026470v2.jpeg)
:quality(80)/p7i.vogel.de/wcms/21/6a/216a1b69d48ac4ef7fe694d4c7791531/0131025888v2.jpeg)
:quality(80)/p7i.vogel.de/wcms/4a/8d/4a8d7b8aa03d413a2bbcf34fdf463306/0131025869v2.jpeg)
:quality(80)/p7i.vogel.de/wcms/23/e2/23e2e753cc718480ede0fadd24e0ee02/0131121023v1.jpeg)
:quality(80)/p7i.vogel.de/wcms/b5/63/b5634bbb6ac68f7f55fb261344d6fa1f/0131163645v2.jpeg)
:quality(80)/p7i.vogel.de/wcms/2b/5e/2b5e4798cb0d86b0f29ba4de833c1412/0131003303v1.jpeg)
:quality(80)/p7i.vogel.de/wcms/54/50/5450b302b2cfe1f29c6f3d5c300123ce/0131004604v2.jpeg)
:quality(80)/p7i.vogel.de/wcms/48/97/4897129d96e4ab9287933406b153ab51/0131163956v2.jpeg)
:quality(80)/p7i.vogel.de/wcms/f6/a8/f6a8a2ac333baa08d168cc68ac2192c0/0131001826v2.jpeg)
:quality(80)/p7i.vogel.de/wcms/34/ff/34ff3de563d63ac821f789f8ca397070/0130971132v2.jpeg)
:quality(80)/p7i.vogel.de/wcms/e7/08/e708baaa36f8929e985dfe5baea8bc68/0130734917v2.jpeg)
:quality(80)/p7i.vogel.de/wcms/a2/bf/a2bf01924b12064f93c6f30be4ca6d7a/0131300118v2.jpeg)
:quality(80)/p7i.vogel.de/wcms/e2/fe/e2fee55c4202eaae5c04383233fa8cf3/0131299511v1.jpeg)
:quality(80)/p7i.vogel.de/wcms/a2/a7/a2a7676a95680bba624b1f5b165c8804/0131298919v1.jpeg)
:quality(80)/p7i.vogel.de/wcms/25/d8/25d8dd47da6179f23914adb6bb448757/0131194053v2.jpeg)
:quality(80)/images.vogel.de/vogelonline/bdb/1710600/1710675/original.jpg)
:quality(80)/images.vogel.de/vogelonline/bdb/1682500/1682579/original.jpg)
:quality(80)/images.vogel.de/vogelonline/bdb/1677000/1677080/original.jpg)
:fill(fff,0)/p7i.vogel.de/companies/5f/3f/5f3f63ceedc78/knf-logo.jpg)
:quality(80)/p7i.vogel.de/wcms/b4/4a/b44abe3996c0f2f2c2e40a23f6a67e1f/0125818584v2.jpeg)
:quality(80)/p7i.vogel.de/wcms/1f/89/1f89ec33f25051fb58ffaecf907661c9/0124984189v1.jpeg)